'I'm not being listened to' - new health plan launched as women say they are still ignored
 BBC
BBCZoe Trafford often had to play the role of agony aunt to her customers. But the hairdresser in Liverpool told the BBC there came a point when the roles had to be reversed - the customers in her salon had to instead listen to her problems.
Zoe has had endometriosis, which can cause severe pain and heavy bleeding, since she was a teenager. For years, doctors told her she just had bad periods.
She first spoke to BBC News in 2022, when a women's health strategy for England was published by the Conservative government.
"You'll be alright, it's just normal," she said doctors would tell her. "But it's not normal – I don't think being in pain is normal."
The 2022 strategy promised to "radically improve" how the health and care system engaged with and listened to all women and girls, and to boost health outcomes.
Four years on, that strategy for improving women's healthcare is being updated by a Labour government.
For Zoe, life has changed dramatically since then - and not for the better. She has had major surgery - her womb and part of her bowel have been removed, and she now has to drain her own bladder using a small tube.
She still feels she is not being heard.
"I'm not being listened to. Basically, I've had the surgery but I'm having more and more complications," she says.
Zoe has had to give up hairdressing because the pain of standing is too much to bear. Meanwhile, there's more endless waiting.
"I'm being passed from from urology to 'gynae' back to the GP, and it's just like I'm in a vicious circle, and no one seems to know what to do with me now," Zoe says.
Responding to Zoe's story, Health Secretary Wes Streeting told BBC Radio 4's Woman's Hour that he accepted there is an "endemic problem" in tackling women's health issues within the NHS.
"I could hear it in Zoe's voice, she has clearly had to fight and battle and is weary from it, and it shouldn't be a fight," he said.
'The system is failing women'
The updated version of the strategy comes against a backdrop of criticism that women's voices are often ignored and marginalised by the NHS.
Streeting said some women have been made to feel like "second class citizens" with their pain treated "as an inconvenience and their symptoms as an overreaction".
In his interview with Woman's Hour, the health secretary described a "culture of medical misogyny, sexism in the NHS, both conscious and unconscious bias", in a system which was "getting disproportionately worse for women".
As a result, Streeting stressed that he wanted overall NHS waiting list numbers to fall more quickly for women, while also seeing an improvement in access to women's health services.
The introduction of a digital NHS service next year, for example, is about "trying to get every bit of the patient journey as fast as possible", the health secretary explained.
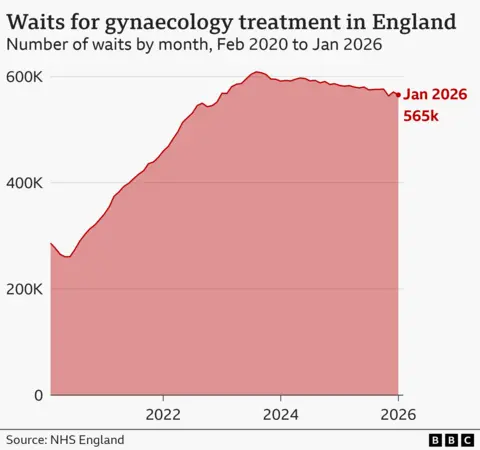
The frustration around delays in accessing healthcare is borne out by the huge rise in the number of women now waiting for gynaecological procedures in England.
BBC analysis shows that between February 2020 and January 2026, the gynaecological waiting list has doubled - increasing to more than half a million (565,000).
This counts the number of waits to start treatment. Some patients could be waiting for more than one treatment.
For all other planned treatment (excluding mental health) waiting lists have risen too - but not by as much (58%).
Among the new measures announced by the government is a new "patient power payment" scheme.
The government says this will enable women to give feedback and report their experiences of treatment. Based on that, money will be allocated to areas needing improvement, and providers getting negative feedback could lose funding.
Gynaecology has been selected for the first trial of the scheme. In future, it could be extended to other health conditions.
There is also going to be a streamlined process for referral to appropriate clinicians with the aim of cutting down long waits for treatment.
And a new standard of care will be introduced to ensure women are offered appropriate pain relief for invasive gynaecological procedures.
Dr Alison Wright, president of the Royal College of Obstetricians and Gynaecologists, welcomed the strategy but said, despite government commitments on waiting lists, "the picture for women remains deeply concerning".
"With over 565,000 women still waiting for gynaecological care, there is a clear opportunity to embed Women's Health Hubs within the neighbourhood health model," she said.
The Royal Osteoporosis Society questioned the strategy, saying there is still no national plan for specialist services for the condition - which affects half of women over 50 and leaves them at risk of hip fractures - despite an earlier government commitment.
Dr Sarah Jarvis, a GP and ambassador for the Royal Osteoporosis Society, said around 2,000 lives were at stake every year "without a clear plan".
A new strategy was "desperately needed", Emma Cox, chief executive of Endometriosis UK, said. She said diagnosis times of more than nine years for endometriosis were "totally unacceptable".
"These commitments must be matched with a clear roadmap for delivery, including ensuring the necessary resources and capacity," she said.
Others feel disappointed. Dr Stephanie Cook, a GP and director of strategy of Women's Health Liverpool, was cautiously optimistic about the strategy four years ago but feels differently now.
"Being honest, I'm disappointed there were so many good ambitions there, but the support just hasn't come," said Dr Cook.
"It just feels like no one's listening. We've got the solutions. We know they work."
The Scottish government recently published phase two of a women's health plan, which was first launched in 2021. This includes transforming services to ensure women and girls have timely access to gynaecological care.
The Welsh government launched a Women's Health Plan in 2024 aiming to "close the gender health gap by providing better health services for women".
In Northern Ireland, authorities have been developing a Women's Health Action Plan.
Additional reporting by Alison Benjamin.
